BRAND INFORMATION
Active ingredient: Liraglutide
Schedule: S4
Class: GLP-1 agonist
Manufacturer: Novo Nordisk Pharmaceuticals Pty
Please read this leaflet carefully before you start using Saxenda.
Even if the needle in your Saxenda® pen has been replaced, do not share it with anybody. You might infect other people or yourself with a serious illness.
What Saxenda® is and what it is used for
Saxenda® is a weight loss medicine that contains the active ingredient liraglutide. Liraglutide is contained in Saxenda®. It’s much like the hormone GLP-1, secreted by the small intestine. One dose of Saxenda® is administered daily.
Saxenda® is used in persons 18 and older who have:
- a BMI above 30 (obese);
- BMI between 27 and 30 (overweight);
- weight-related health concerns (diabetes, high blood pressure, abnormal blood lipids, sleep apnea).
You should have lost at least 5% of your starting weight after 12 weeks of using Saxenda at a 3.0 mg/day dose. To get long-term care, you must see a physician. Saxenda® should be taken in addition to a healthy diet and regular exercise.
BMI calculates a person’s weight in relation to height. It’s calculated by dividing weight by height squared.
Body Mass Index Calculator
?
BMI is calculated by dividing your weight in kilograms by your height in metres squared.
Enter your measurements and click ‘calculate’ for your body mass index.
If your BMI is above or below the normal range but you consider yourself to be of normal and healthy weight for your height, chat with your doctor about any potential health concerns.
This calculator has been reviewed by NeverGiveUpTeam experts and is based on reputable sources of medical research. It is not a diagnostic tool and should not be relied on as a substitute for professional medical or other professional health advice.
Saxenda® suppresses your appetite by binding to hunger-regulating brain receptors. So you’ll be able to eat less and shed pounds. Also, Saxenda® helps you keep the weight off and prevent gaining it back after losing it.
- Children and teens under 18 should not take Saxenda®. Because the drug’s effects on this age range are unknown.
- Saxenda® is not addictive.
- Saxenda® is available only with a doctor’s prescription.
Before you start to use it
During Saxenda® therapy, tell your doctor if you have:
- diabetes (Saxenda® shouldn’t replace insulin; s axenda® and insulin are incompatible);
- cardiac failure (If you have severe heart failure, don’t use Saxenda®);
- prescription for any weight loss meds, OTC, or natural weight-loss drugs;
- Crohn’s disease;
- gastroparesis;
- thyroid disease, including nodules and enlargement.
- renal disease/dialysis;
- liver issues;
- pancreatitis;
- depression, suicidal thoughts, or another mental disorder;
- gained weight due to medical issues or medications.
Before beginning Saxenda®, make sure you have enough water in your system. Dehydration causes renal issues requiring dialysis. When in doubt, consult your doctor.
If you get significant upper abdominal pain, particularly on the right side, stop taking Saxenda® and see a doctor. Back or right shoulder pain is possible. Gallstones and gallbladder inflammation may occur as a result of weight loss.
Saxenda® hasn’t been thoroughly tested in people beyond 75 years of age. So people above the age of 75 should avoid the drug.
Allergy warnings should be included in your medical history.
Inform your primary care provider if you are or intend to become pregnant. Research on the drug’s impact during pregnancy is lacking. Saxenda® is not recommended for pregnant women. Saxenda® may harm a fetus.
Are you currently nursing a baby, or do you intend to do so in the future? Make an appointment with your doctor to discuss this matter. It is not known if Saxendabreast ® passes through milk. Saxenda® should not be taken by breastfeeding women.
Before using Saxenda, tell your doctor if you have any of the conditions mentioned above.
Precautions
See also the Warning section.
Before using liraglutide, tell your doctor or pharmacist if you are allergic to it; or if you have any other allergies. This product may contain inactive ingredients, which can cause allergic reactions or other problems. For further information, speak with your pharmacist.
Make sure you notify your doctor or dentist about all the prescription, nonprescription, and herbal products you use before undergoing any procedure.
If you have diabetes, this product may affect your blood sugar. Check your blood sugar regularly as directed and share the results with your doctor. If you see signs of low blood sugar, contact your doctor immediately (see Side Effects section). The medicine your doctor has prescribed for your diabetes may need to be adjusted, as well as an exercise program, or diet.
Pregnant women should not use this medicine. Unborn children may be harmed by it. Tell your doctor straight away if you get pregnant or suspect you may be pregnant.
Whether this drug is excreted in breast milk is still a question mark. Before you start breastfeeding, make an appointment with your doctor. Consult your pharmacist or physician.
Interactions
Interactions between drugs might alter their effectiveness or raise your vulnerability to harmful side effects. All probable medication interactions are not included in this text. Your doctor and pharmacist will be able to help you if you keep a list of all the items you use (prescription and over-the-counter). Unless directed otherwise by your physician, never start, stop, or alter the dose of any medications.
Some products that may interact with this drug include diabetes medications (such as insulin, sulfonylureas including glyburide).
Do not use this drug with any other product containing liraglutide or other medications similar to this medication but used for diabetes (such as exenatide and dulaglutide).
Taking other medicines
Your doctor or pharmacist will need to know whether you’re taking any additional medications, including those purchased over the counter at your pharmacy, supermarket, naturopath, or health food store.
In particular, tell your doctor or pharmacist if you are using medicines:
- for treating type 2 diabetes, such as sulfonylurea (including glimepiride or glibenclamide). You may get low blood sugar (hypoglycaemia) when you use these medicines with Saxenda®. Your doctor may adjust the dose of your diabetes medicine to prevent you from getting low blood sugar.
- to thin your blood (anticoagulants), such as warfarin or other types of medicines called ‘coumarin derivatives’. Your doctor may need to monitor you more closely.
- for high blood pressure, such as amlodipine, atenolol or bisoprolol or for heart disease, such as digoxin.
- for HIV, such as atazanavir or ritonavir.
Also, be sure to let your doctor know if you’re taking any additional medications. This can’t be stressed enough. Your doctor’s job is to tell you whether or not to continue taking them.
Both your physician and pharmacist can help.
Do not use Saxenda® if:
- you or any of your family have ever had MTC or if you have MEN 2.
- you are allergic to liraglutide or any of the ingredients in Saxenda®.
- you are pregnant or plan to become pregnant. Saxenda® may harm your unborn baby
How to use Saxenda®
You should have received instructions on how to take your medication from your physician or pharmacist. Observe all the instructions. There is a possibility that the info in this leaflet is different.
A doctor, nurse, or pharmacist may explain the directions if necessary.
You’ll be put on a diet and fitness plan by your doctor. Maintain your participation in this program while taking Saxenda®.
If your doctor does not provide sufficient information about your eating, you may choose to opt for a customized Saxenda meal plan (Australia). Make sure that it fits your daily needs for the necessary elements.
Saxenda® is supplied as a pre-filled pen containing liraglutide. The Saxenda® pen can give doses of 0.6 mg, 1.2 mg, 1.8 mg, 2.4 mg or 3.0 mg.
How much to use
Your doctor will tell you how much of this medicine you need to use each day.
- The usual starting dose is 0.6 mg once a day.
- Your doctor will tell you how long to keep taking this dose. It will be for at least one week.
- Your dose may then be increased by 0.6 mg each week until you reach the recommended dose of 3.0 mg once a day.
- Your doctor will tell you how much Saxenda® to use each week. Usually, you will be told to follow the table below:
| Week | Dose to inject |
| 1 | 0,6 mg once a day |
| 2 | 1,2 mg once a day |
| 3 | 1,8 mg once a day |
| 4 | 2,4 mg once a day |
| 5 onwards | 3,0 mg once a day |
Once you’ve reached the 3.0 mg dosage in week five of therapy, stick with it until the completion of the treatment term. The dosage should not be increased anymore.
Visit your doctor frequently to see whether Saxenda® therapy is still necessary for you. A doctor’s prescription is required for any dosage adjustments.
When to use it
You can use Saxenda® at any time of day, with or without food and drinks. It is preferable to use Saxenda® at about the same time each day, at a time that is most convenient for you.
Speak to your physician or go to the nearest hospital if you think that you are using Saxenda® excessively. Carry the medical bag with you. You might be in need of medical care. If you take too much Saxenda®, you may have nausea, vomiting, or low blood sugar (hypoglycaemia). Hypos can be detected early if you observe the symptoms listed below.
- Don't inject Saxenda with other drugs (e.g. insulins).
- Do not combine Saxenda® with GLP-1 receptor agonists (e.g. exenatide or lixisenatide).
If you forget to use it
Within 12 hours after forgetting a dosage, inject Saxenda® as soon as you realize you haven’t taken it.
If, on the other hand, it has been more than 12 hours since you were supposed to use Saxenda®, you should omit the missed dosage and re-inject it the following day at the regular time.
To make up for a missed dose, do not utilize an additional dose or raise the dosage the next day.
Ask your doctor, nurse or pharmacist for advice if you’re unclear of what to do.
While you are using Saxenda®
Must-dos
Tell your doctor if you have diabetes. Your physician may change your diabetic medication to avoid ‘hypos’ (low blood sugar levels).
- Don't inject Saxenda with other drugs (e.g. insulins).
- Do not combine Saxenda® with GLP-1 receptor agonists (e.g. exenatide or lixisenatide).
Travelling? Tell your doctor, nurse, or pharmacist. Request a letter outlining why you’re bringing injectables. You should carry several copies of this letter to each state you visit.
Your destination country may not have Saxenda®. A doctor, nurse, or pharmacist can give you helpful tips.
Things you must not do
- Do not stop taking your medication until instructed.
- Do not use this medicine if you think it has been frozen or exposed to excessive heat.
- Use this drug just as your doctor directs.
- Even if others have the same ailment, don't share your medication.
- Do not share needles or pens.
Things to be careful of
Drive carefully until you know how Saxenda® affects you. Consult your doctor or pharmacist for details.
Side effects
If you get ill while taking Saxenda®, call your doctor, nurse, or pharmacist right away. The side effects of any medicine are a given. In most cases, they’re not so severe. However, adverse symptoms may need a trip to the hospital for evaluation and treatment.
Don’t be alarmed by these side effects; they can disappear soon. Don’t hesitate to ask your doctor, nurse, or pharmacist if you have any questions.
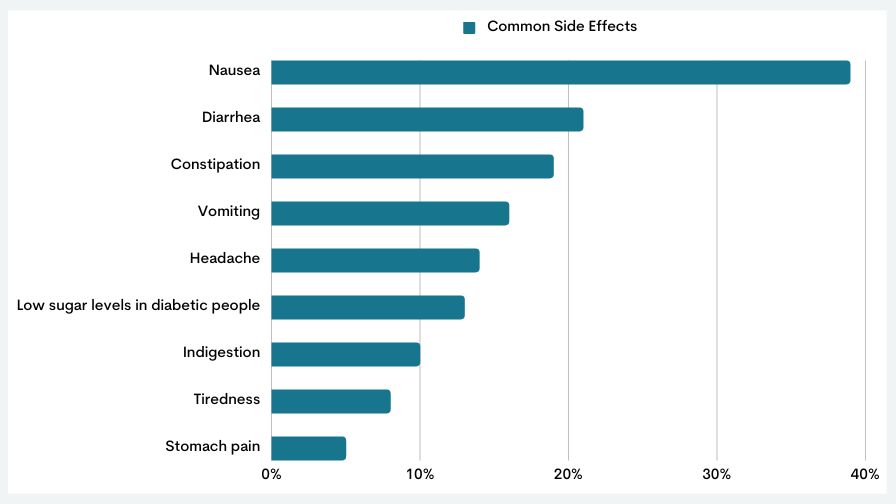
Saxenda® often causes:
- nausea;
- vomiting;
- diarrhoea;
- constipation;
- headache.
These are mild side effects that lessen with regular drug usage.
If any of the following concerns you, see your doctor:
- changed sense of taste;
- dizziness;
- indigestion (dyspepsia);
- bloating, burping, gas, dry mouth;
- heartburn;
- abdominal pain/swelling;
- hypoglycemia;
- injection site reactions (bruising, pain, irritation, itching and rash);
- tachycardia;
- fatigue;
- sleeplessness (insomnia).
These symptoms might occur in the first 3 months of therapy.
This list contains typical pharmaceutical side effects – mild and temporary.
Less common side effects:
- feeling bad overall;
- hives (a type of skin rash);
- loss of fluids (dehydration);
- (dehydration).
This may be caused by vomiting, nausea, and diarrhoea at the beginning of therapy.
Hypos are more common in diabetics receiving sulfonylurea. Hypo may strike abruptly. Hyposymptoms include:
- pale skin, chilly sweat;
- headache;
- tachycardia;
- nausea;
- feeling famished;
- vision changes;
- sleepiness;
- feeling weak, frightened, or confused;
- difficulties with concentration;
- rattle (tremor).
Your doctor can tell you how to manage low blood sugar and what to do if you have these symptoms. If you’re taking sulfonylurea when you start Saxenda®, your doctor may cut the dosage.
Tell your doctor immediately if you:
- have nausea, vomiting, and intense stomach discomfort that may spread to your back. A potentially fatal illness known as pancreatitis may cause this complication. Stop taking Saxenda® if this occurs.
- get a lump or swelling in your neck, hoarseness, trouble swallowing, or shortness of breath.
- have complaints such as decreased urine output, a metallic aftertaste, and a tendency to bruise easily. All that points to impaired kidney function.
- feel upper right side abdominal pain, yellowing of the skin and eyes or clay-coloured stools, which may be signs of gallbladder problems.
- experience depression or mental changes that are new, severe, or worrying.
Tell your doctor if you notice anything else that is making you feel unwell.
Inform your doctor immediately or go to Accident and Emergency at your nearest hospital if you notice any of the following:
- skin rashes over a large part of the body;
- shortness of breath, wheezing;
- swelling of the face, lips or tongue;
- fast heartbeat;
- sweating.
There are a number of dangerous symptoms on this list that may indicate an allergic response of some kind. You may need to be admitted to the hospital or get emergency medical care. Fortunately, these adverse effects are quite uncommon.
Some individuals may have additional side effects that aren’t included here.
Ask your doctor, nurse, or pharmacist if you have any questions about your medical care.
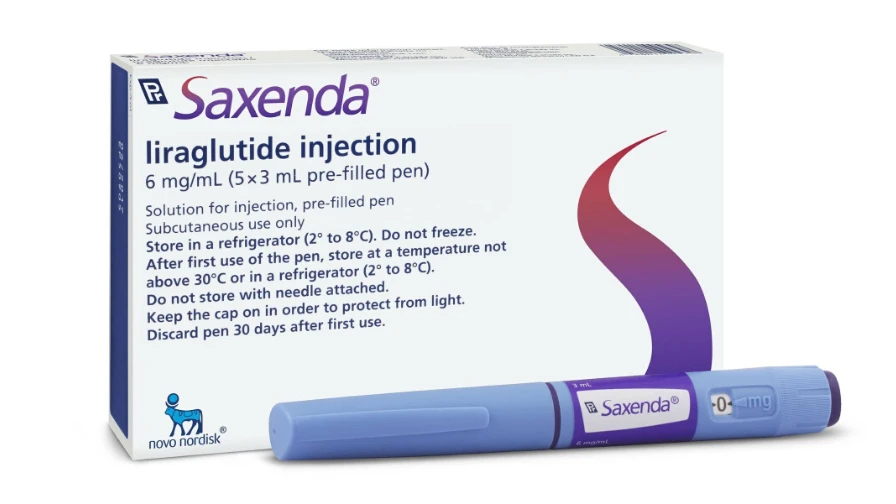
Product description
What it looks like
Each pen contains 3 mL of solution and is able to deliver doses of 0.6 mg, 1.2 mg, 1.8 mg, 2.4 mg or 3.0 mg.
Saxenda® is available in packs containing 1, 3 or 5 pens.
Not all pack sizes may be marketed.
This medicine is a colourless, clear injection
Needles are not included.
Color: colourless, clear injection solution
Ingredients
Saxenda® contains liraglutide (rys) 6 mg/mL as the active ingredient. The abbreviation ‘rys’ indicates the method of genetic engineering used to manufacture the liraglutide.
Saxenda® also contains the following inactive ingredients: dibasic sodium phosphate dihydrate, propylene glycol, phenol, hydrochloric acid, sodium hydroxide and water for injections.
Supplier/Sponsor
Location | Australia | New Zealand |
Company | Novo Nordisk Pharmaceuticals Pty. Ltd. | Novo Nordisk Pharmaceuticals Ltd. |
Address | Level 10 118 Mount Street North Sydney NSW 2160 | 58 Richard Pearse Drive Airport Oaks Mangere |
Australian Registration Number:
AUST R 225804
Saxenda®, NovoFine® and NovoCare® are trademarks owned by Novo Nordisk A/S.
© 2021
Novo Nordisk A/S
Further information
The Australian ‘Product Information’ document is available from the following websites:
www.novonordisk.com.au
https://www.ebs.tga.gov.au/
For further information, call the NovoCare® Customer Care Centre on 1800 668 626 or 0800 733 737 (NZ).
www.novonordisk.com.au
www.novonordisk.co.nz
further dietary advice, refer to the dietary guidelines on the NH&MRC website at www.nhmrc.gov.au (Australia), or the current food and nutrition guidelines on the Ministry of Health website at www.health.govt.nz (New Zealand).
References
- Saxenda. Available from: [URL Link]
- Saxenda Subcutaneous: uses, side effects, and more. WebMD. Available from: [URL Link]
- Saxenda – NPS Medicinewise. Available from: [URL Link]
- Saxenda (liraglutide) injection 3 mg savings card, Novocare. Available from: [URL Link]
- Using the Saxenda® Pen. novomedlink.com. Available from: [URL Link]
- Saxenda (liraglutide) injection 3 mg. Official physician site. Available from: [URL Link]
- Saxenda: uses, dosage, and side effects. Available from: [URL Link]
- Saxenda 6 mg/mL solution for injection in pre-filled pen. Available from: [URL Link]
- Saxenda (liraglutide): basics, side effects &reviews. Available from: [URL Link]
- Saxenda. European Medicines Agency. Available from: [URL Link]
- Saxenda. Healthdirect. Available from: [URL Link]
FAQ about Saxenda (liraglutide)
Weight loss normally starts within 2 weeks of starting Saxenda (liraglutide).
Upon stopping Saxenda (liraglutide), some people will likely regain the lost weight. Keeping a healthy weight requires close collaboration with your healthcare professional.
It is not a type of insulin, but it can impact the amount of insulin your body releases. This medication is also available as Victoza (liraglutide) for diabetes.
The injection should be given at the same time every day. You may inject it whenever is most convenient for you (such as before breakfast, lunch, dinner, or sleep).
Most of the side effects may go away during treatment as your body adjusts to the medication.
Healthdirect is not for emergency usage. Call triple zero (000) if you have an acute sickness, overdose, or emergency.
When created, correct information was provided. This material shouldn’t be used to replace medical advice, diagnosis, or treatment. Please see our terms and conditions.










My body adjusted to it only after A MONTH. This drug is for patient ones.
The fitness part is very important for that drug to work. Without it, you will just lose your time.
I remember I hated the idea of taking a pill for weight loss. But unfortunately, nothing else worked for me. Now I’m happy I tried.
The hardest part here is to give an injection correctly. All the rest went good for me. I’ve shed extra pounds rather quickly without severe adverse effects.
Taking Saxenda was one of the most horrible experiences in my life. I had diarrhea for a week and couldn’t even work properly. Had to quit the drug cause I’m not planning to live in the bathroom.
I wanted to try this one, but there is a history of thyroid disease in my family((. Be careful about precautions and always consult your doctor.
I’m about to start taking Saxenda, and this info was helpful. Thanks
It’s a number one weight loss drug for me. Almost no side effects (except for nausea at first). I’ve lost 10 kg in 3 months thanks to it. I didn’t do any workouts and stuff like that.